Carotid endarterectomy may be performed if you have had a TIA (mini-stroke), a sudden loss of vision in one eye, or a major stroke. This is due to carotid artery disease; the narrowing of the main artery to your brain in your neck. The danger is that you may suffer another major stroke in the future.
In a small number of people a tight narrowing is discovered whilst under investigation for another problem. If this applies to you, you will still undergo the same preoperative tests, but you will be admitted to hospital electively for surgery.
The aim of carotid endarterectomy is to prevent you having a major stroke. The following information will help explain the process of a carotid endarterectomy operation.
Before the treatment
Your stay in hospital
The operation
Recovery and aftercare
Complications
How you can help yourself
Before the treatment
Before you have carotid surgery, there are a number of tests that need to be done to assess whether you are able to have the operation, and some immediately before the surgery (pre-operative tests).
Tests to see whether you are suitable for the operation include:
- Ultrasound scan MRA or a dye X-ray (digital subtraction angiogram) of the arteries
- Blood tests
- ECG (a heart tracing)
- Echocardiogram (an ultrasound test of the heart)
- Breathing test
- CT scan (special X-ray scan) of your brain.
You may also have a special MRI scan of your brain at the same time as the MRA.
These tests should have been done within a couple of days of your symptoms. If you are fit enough, you will then be offered an operation within two weeks of your symptoms.
Your stay in hospital
You should bring with you all the medications that you are currently taking. You should continue to take your normal medication prior to the operation unless instructed otherwise.
You will be admitted to your bed by one of the nurses who will also complete your nursing record.
You will be visited by the surgeon who will be performing your operation, and also by the doctor who will give you the anaesthetic.
Physiotherapists and Intensive or High Dependency Care staff may also visit, to give you information about your postoperative care. If you have any remaining questions about the operation please ask the doctors.
You will be asked to sign a form confirming that you understand why the procedure needs to be performed, the risks of the procedure and that you agree to the surgery.
The operation - the anaesthetic
Carotid endarterectomy can be performed under either regional (local) or general anaesthetic. Not all cases are suitable for regional anaesthetic and not all hospitals are able to offer this service. Your surgeon will advise you as to which method of anaesthetic you will be offered.
For a general anaesthetic, a tiny needle is placed in the back of your hand. The anaesthetic is injected through the needle and you will be asleep within a few seconds.
For local anaesthetic, the anaesthetist will make an injection into the skin of your neck to numb it. During the operation, if you become uncomfortable, the surgeon will inject more local anaesthetic. You will also be given some sedation, and as a result, you may not be very aware of the operation at all. Occasionally it may be necessary to convert to a short general anaesthetic during the operation.
A tube (catheter) may be inserted into your bladder to drain your urine.
A drip is placed into a vein in your arm (wrist usually) to give you some fluids during and following surgery. Sometimes, a second drip will be placed into an artery at wrist level to permit careful blood pressure monitoring during and just after the operation.
The operation
You will have a cut running vertically down from near the angle of your jaw / ear lobe towards your breastbone. The incision is usually 7-10cm in length.
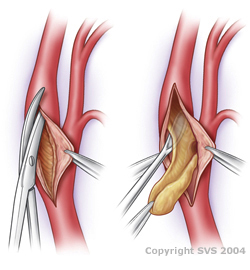
Once the carotid artery is displayed, the branches of the artery are clamped to limit blood loss during the operation. A small incision is made along the artery and the plaque or narrowing is carefully removed.
When the inside of the artery has been cleared, it is closed with very fine stitches. A small patch will usually be stitched to the artery to prevent further narrowing. This patch is normally made of a material called Dacron, but sometimes a vein from your leg may be used or a piece of animal tissue (bovine).

The wound is usually closed with a stitch under the skin that dissolves.
To protect the brain from interruption to its blood supply while the artery is clamped, a shunt (narrow plastic tube) is sometimes used to maintain blood flow. The shunt lies in a loop outside the artery, passing into the artery above and below at each end of the incision in the artery.
To monitor the blood supply to your brain a special listening device may be placed onto your head. This allows the surgeon to hear and see how fast your blood is running, which will help them make decisions during the operation.
At the end of the operation your surgeon may look inside the artery with a special camera to check that the repair is satisfactory and that there is no blood clot.
Your surgeon may place a small plastic drain in your neck for a short period to look for bleeding and to reduce neck swelling after the operation.
Recovery and aftercare
You may be taken to the High Dependency Unit for up to 24 hours after your operation so that your progress can be closely monitored.
You will wake up immediately at the end of the operation (if it has been under general anaesthetic). Local anaesthetics are used to numb the skin in all cases so there should be little discomfort.
Following this sort of surgery you are unlikely to feel sick, and you should be able to eat and drink again within a few hours. Your mobility will return to normal more or less immediately.
There is often some swelling in the neck, but this settles within 7-10 days.
The incision on your neck will initially be very visible; however this will subside and become virtually invisible within 2-3 months.
A blood transfusion is rarely required.
Going home
Most people stay in hospital between 2 and 4 days after carotid endarterectomy.
If your stitches or clips are the type that need removing this is usually done whilst you are still in hospital. If not, it will be arranged for your GP’s practice or district nurse to remove them and check your wound.
Regular exercise such as a short walk combined with rest is recommended to provide a gradual return to normal activity.
Driving: You will be able to drive when you can perform an emergency stop safely and look over your shoulder easily. This will normally be 2-3 weeks after surgery, but if in doubt check with your own doctor. You should inform your insurers that you have had this operation.
Bathing: Once your wound is dry after 3-4 days you may bathe or shower as normal.
Work: If this applies to you, you should be able to return to work within 3-4 weeks of surgery. Your GP will advise you of this when you see him/her for your sick-note.
Lifting: There are no limitations in this area.
Medicines: You will usually be sent home on a small dose of aspirin if you were not already taking it. This makes the blood less sticky. If you are allergic to aspirin, or if it upsets your tummy, an alternative drug may be prescribed. No other changes to your medication are required.
Complications
Stroke: A small number of people, between 1 and 3 in 100, having carotid endarterectomy will have a stroke during the operation. The severity of stroke can be very mild causing little or no disability, through to severe causing major disability and death. All possible precautions will be taken to prevent this eventuality.
Other major complications: As with any major operation there is a small risk of you having a medical complication such as a heart attack, kidney failure, chest problems or infection in the wound. Each of these is rare, but overall it does mean that some patients may have a fatal complication from their operation. For most patients this risk is about 2% - in other words 98 in every 100 patients will make a full recovery from the operation.
If your risk of a major complication is higher than this, usually because you already have a serious medical problem, then your surgeon will discuss this with you. It is important to remember that your surgeon will only recommend treatment if he or she believes that the threat of stroke without operation is much higher than the threat posed by the operation itself.
Chest infections: These can occur following this type of surgery, particularly in smokers and may require treatment with antibiotics and physiotherapy.
Wound infection: Wounds sometimes become infected and this may need treatment with antibiotics. Wound infections for this type of procedure are rare. Infection of the inserted patch is a very rare, but serious complication.
Fluid leak from wound: The wound can bleed which may lead to swelling. Usually the swelling will settle on its own, but occasionally the wound may need further surgical attention. If you have been started on tablets to thin your blood when you were admitted for symptoms of TIA or stroke, then you may be at an increased risk of bleeding that may require a return to theatre.
Nerve injuries: These are uncommon. Skin nerves are interrupted by the incision leading to some loss of skin sensation, which may recover over time. Movement of nerves nearer the carotid artery can lead to temporary or rarely permanent loss of function. The vagus nerve provides a branch to the voice box (larynx) leading to a hoarse sounding voice. The hypoglossal nerve supplies the muscles of the tongue affecting speech slightly by reducing the tongue’s mobility. The facial nerve supplies the muscles of the face; damage to its lowest branch may lead to impaired movement of muscles around the lower jaw and neck.
How you can help yourself
If you are a smoker you should make a determined effort to stop completely. Continued smoking will cause further damage to your arteries and increases the risks of heart attacks, strokes, and problems with the circulation in your legs.
You should eat a low fat diet, avoiding food with high saturated fat content and take regular exercise.
More information and advice about vascular health.
Whilst we make every effort to ensure that the information contained on this site is accurate, it is not a substitute for medical advice or treatment, and the Circulation Foundation recommends consultation with your doctor or health care professional.
The Circulation Foundation cannot accept liability for any loss or damage resulting from any inaccuracy in this information or third party information such as information on websites to which we link.
The information provided is intended to support patients, not provide personal medical advice.